CIAs, Exclusions, and Your Practice
Guest Author: Rachel V. Rose, JD, MBA
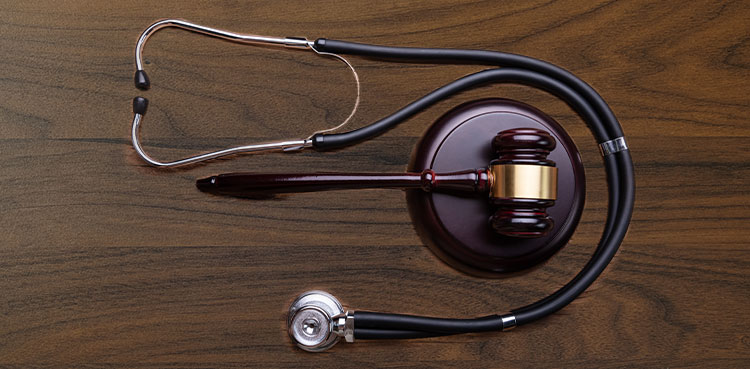
Contracting with or employing an excluded person can result in a government enforcement action.
Before delving into a recent U.S. Department of Justice (DOJ) settlement, which involved employing an “excluded” individual, it’s important to appreciate some of the tools that the U.S. Department of Health and Human Services Office of the Inspector General (HHS-OIG) has at its disposal – corporate integrity agreements (CIA) and exclusion from all federal programs.
CIAs – are negotiated by HHS-OIG “with healthcare providers and other entities as part of the settlement of Federal health care program investigations arising under a variety of civil false claims statutes. Providers or entities agree to the obligations, and in exchange, OIG agrees not to seek their exclusion from participation in Medicare, Medicaid, or other Federal health care programs.” Typically, a CIA lasts 5 years and the person who enters into the CIA must make scheduled reports to HHS-OIG. Importantly, CIAs are specific to the facts and circumstances of a particular matter and include breach and default provisions, which enable HHS-OIG to impose additional monetary penalties (i.e., Stipulated Penalties). A material breach of the CIA “constitutes an independent basis for the provider’s exclusion from participating in Federal healthcare programs.”
Exclusions – have been around since 1977 and are imposed by HHS-OIG; however, they may arise because of a False Claims Act case or other matter that was initiated through or by DOJ. HHS-OIG’s authority to impose exclusions is derived from the Social Security Act §§ 1128, 1156.“The scope of an exclusion under section 1128 of the Act is from all Federal health care programs, as defined in 42 CFR 1001.2. … Exclusions under section 1156 of the Act do not reach other Federal programs (although HHS or another Federal agency could separately initiate a suspension or debarment of an excluded person from other Federal procurement or nonprocurement programs).” The process begins when a person receives a Notices of Intent to Exclude (NOI). From there, the recipient of the NOI is given the opportunity to respond. Once all the information is considered, HHS-OIG renders its decision. If the findings substantiate exclusion, the person is notified. From there, they may appeal to an HHS Administrative Law Judge and further appeal to the HHS Departmental Appeals Board (DAB). After the DAB renders its decision, judicial review in a U.S. District Court is also available. Reinstatement of an individual or entity is not automatic; rather, the person must apply for reinstatement. If reinstated, the person receives written notice from HHS-OIG that they have been reinstated. The excluded individual may begin the process 90 days before their period of exclusion ends.
On March 18, 2022, the DOJ announced that Windham Eye Care Practice and its Owners Pay $192K for Employing “Excluded” Individual. Specifically, the federal and state governments entered into a civil settlement agreement “to resolve allegations that they improperly employed an individual who was excluded from all federal healthcare programs.” Windham Eye Group (WEG) employed Michael Vallone as its practice administrator from February 2010 through May 2021. Previously, Mr. Vallone was convicted of healthcare fraud in the District of New Jersey and was excluded from all federal healthcare programs under §1128 of the Social Security Act.
As noted by the DOJ, when HHS-OIG “excludes an individual or entity from federal health care programs, no program payments may be made for items or services furnished by that excluded individual or entity.” (emphasis added). The relevance to the WEG was that a portion of the reimbursements received from the federal healthcare programs were used to pay Mr. Vallone’s salary and benefits.
I have often reiterated the phrase, “an ounce of prevention is worth a pound of cure.” HHS-OIG issued an Updated Special Advisory Bulletin in May 2013, emphasizing that in order to avoid potential liability, health care providers and organizations providing services directly or indirectly should check the List of Excluded Individuals/Entities on the HHS-OIG website. It is imperative that entities receiving remuneration from Federal health care programs – whether directly or indirectly, have both background checks and exclusion checks as part of their policies and procedures.
 About the Author
About the Author
Rachel V. Rose, JD, MBA, advises clients on compliance, transactions, government administrative actions, and litigation involving healthcare, cybersecurity, corporate and securities law, as well as False Claims Act and Dodd-Frank whistleblower cases. She also teaches bioethics at Baylor College of Medicine in Houston. Rachel can be reached through her website, www.rvrose.com.
Originally posted on: physicianspractice.com




