Meaningful Use Ends In 2016?
Due to the challenges of implementing Meaningful Use, it is unsurprising the Center for Medicare and Medicaid Service (CMS) is finally rethinking the plan. The goal of Meaningful Use (MU) to achieve nationwide electronic health record (EHR) interoperability and ultimately improve overall healthcare remains intact. Until further details and a formal announcement, certain steps will be necessary.
CMS administrator Andy Slavitt’s following announcement at the J.P. Morgan Healthcare Conference on January 12, 2016 gave some insight into the future of the program: “Now that we effectively have technology into virtually every place care is provided, we are now in the process of ending Meaningful Use and moving to a new regime culminating with the Medicare Access and CHIP Reauthorization Act (MACRA) implementation. The Meaningful Use program as it has existed, will now be effectively over and replaced with something better.”
Details are to be announced over the next several months but the focus will include:
- Rewarding providers for patient outcomes not use of technology;
- Customizing goals for provider’s practice, user-centered and supporting not distracting physician;
- Requiring open API’s to get data in and out of EHR securely; and
- Focusing on interoperability and engaging patients in their care.
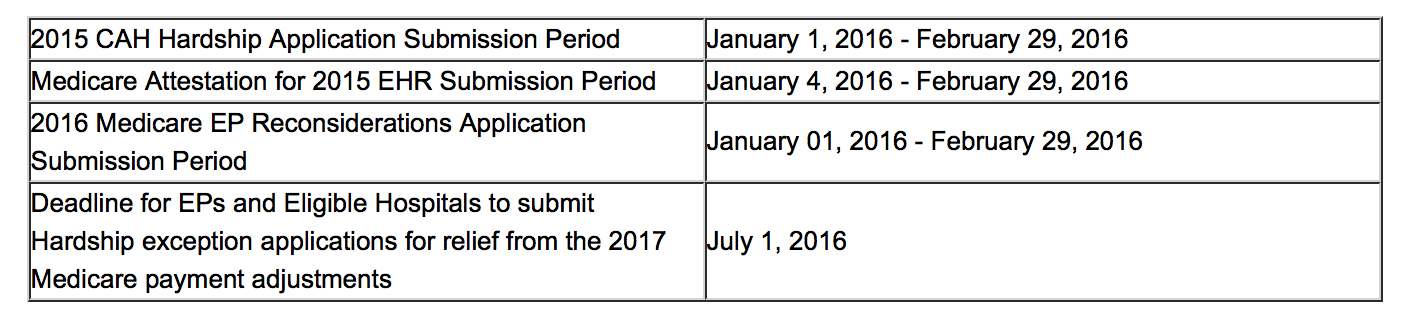
While waiting for further details and a formal announcement from CMS, deadlines will still need to be met for Meaningful Use.
What is EHR interoperability?
EHR interoperability is the ability to exchange medical and treatment information from provider to provider with the receiving provider’s EHR integrating the exchanged information into their system. Specifically, providers should be able to:
- View results from diagnostic procedures conducted by other providers to avoid duplication;
- Evaluate test results and treatment outcomes over time regardless of where the care was provided to better understand a patient’s medical history;
- Share a basic set of patient information with specialists during referrals and receive updated information after the patient’s visit with the specialist to improve care coordination;
- View complete medication lists to reduce the chance of duplicate therapy, drug interactions, medication abuse, and other adverse drug events; and
- Identify important information, such as allergies or preexisting conditions, for unfamiliar patients during emergency treatment to reduce the risk of adverse events.
Ongoing Challenges of Meaningful Use
What are the obstacles preventing Meaningful Use from improving the quality and efficiency of healthcare and patient safety? A study by the Government Accountability Office (GAO) in September 2015 outlined the 5 biggest challenges to the success of EHR interoperability:
- Insufficiencies in health data standards;
- Variation in state privacy rules;
- Accurately matching patient’s health records;
- Costs associated with interoperability; and
- Need for governance and trust among entities such as agreements to facilitate sharing information.
A data format standard for EHR, Consolidated Clinical Document Architecture (C-CDA) has been used by most of the health information technology industry however the methods of implementation and use of terminology are varied. Due to this variation, the receiving provider’s EHR may not be able to view the information exchanged.
Even more problematic are state regulations. Some states do not allow for automatic sharing in the health information exchange. A patient must consent to opt in or in some states patients are permitted to opt out. Additional consent requirements that are state-specific for sensitive information such as HIV or mental health records may not be adequately separated from the remainder of the record to avoid disclosure. These state specific variations would be difficult to navigate for complete EHR interoperability.
Accurately matching patient records may be difficult if the demographic identifiers used are varied amongst providers. In the case of similar demographic information among patients such as name, specific criteria will need to be met to accurately distinguish these individuals.
Cost still remains a major problem for the providers to achieve interoperability. Additional fees may be necessary for customized interfaces and any legal fees would also be the responsibility of the providers.
Organizational policies on privacy, security, data use and technical standards may vary between entities. Addressing these policy differences would be necessary to facilitate information sharing between entities.

